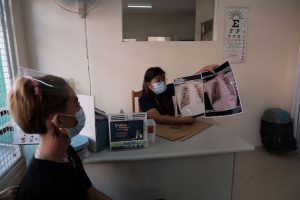
A doctor talks to a TB survivor at a clinic in Manilla,
Philippines. Credit: Getty Images for TB Alliance
By Ed Holt
BRATISLAVA, May 2 2023 – While there is no established causal relationship between climate change and tuberculosis (TB), studies have begun to highlight the potential impact its effects could have on the spread of the disease.
Undernutrition, HIV/AIDS, overcrowding, poverty, and diabetes have all been identified as TB risk factors that are worsened by climate change. Worryingly, many countries with high burdens of TB, including, for instance, drought-hit Ethiopia, Indonesia, Kenya, and Peru, have suffered from the kind of extreme weather associated with a heating planet.
But despite vying with COVID-19 for the grim distinction of the world’s deadliest infectious disease, claiming 1.6 million lives in 2021, TB is not often talked about in connection with climate change, with the link often overlooked by policymakers.
TB experts say this must change as the climate crisis accelerates.
“The effects of climate change, such as its impact on migration, for instance, are getting attention. What we want to see is for that attention to also get drawn to its effects on TB,” Maria Beumont, Chief Medical Officer at TB Alliance, a global nonprofit organisation developing TB drugs, told IPS.
In recent years, disease experts and climatologists have sounded increasingly dire warnings about the potential impact of the climate crisis on the spread of lethal diseases.
The latest report from the Intergovernmental Panel on Climate Change (IPCC) warned of the health impacts of global heating, including an increase in the incidence of infectious diseases. Meanwhile, other research has shown how changes in climate have aggravated the risks of hundreds of infectious diseases worldwide.
But much of the discussion around that has focused on how higher temperatures and increased incidence of flooding and drought could drive more vector, food and water-borne diseases with diseases.
What has often been overlooked in these conversations, say Beumont and others, is how the effects of the climate crisis could worsen what is de facto a global TB pandemic.
Part of this is because of the nature of those effects in relation to TB.
“The potential impact of climate change [on TB] is more indirect than with some other infectious diseases,” Dr Mohammed Yassin, Senior Disease Advisor, TB, at the Global Fund to Fight AIDS, Tuberculosis and Malaria, told IPS.
TB experts point to how more frequent and more devastating natural disasters linked to climate change, or simply places on the planet becoming too hot to be habitable, are leading to mass displacement, which can create ideal conditions for TB to spread.
“Mass displacement can lead to overcrowding and poor living conditions of those displaced. If some of those people already have symptoms of TB, there is a higher chance of it spreading. There would also be people living under stress, and facing malnutrition, which are factors adding to the potential for TB to spread,” said Yassin.
Displacement also raises issues with access to healthcare for the displaced, which can negatively affect the management of treatment for those with TB because patients need to take treatment daily. Interruption of treatment can leave them infectious for longer and at risk of developing drug-resistant TB, which in turn is much more difficult and expensive to treat.
But displacement would also impact the treatment of those with other conditions, such as HIV and AIDS and diabetes, which weaken immune systems and leave people more susceptible to TB.
Meanwhile, displaced people are likely to find themselves living in crowded areas where, in the absence of adequate screening and diagnostic procedures, TB could spread.
But displacement is far from the only problem. Both extreme droughts and flooding can impact food security, devastating crops and killing livestock and leading to malnutrition and undernutrition—known risk factors for TB.
The impact of extreme weather on health, particularly TB, is already being seen in some parts of the world.
Somalia is in the grip of severe drought following five consecutive failed rainy seasons—something which the UN has said has not been seen for four decades—with five million people facing acute food shortages and nearly two million children at risk of malnutrition, according to the UN.
TB is a major cause of death in Somalia, and late last year, with TB services largely non-existent in settlements for displaced persons, the Global Fund committed USD 1.9 million for food support for thousands of TB patients and outreach activities in settlements. Officials at the time emphasised the importance of such action to help reach the most vulnerable and stop TB from spreading.
Meanwhile, the devastating floods in Pakistan last year, which affected an estimated 33 million people, not only brought an immediate threat of diseases such as malaria and dengue but interrupted vital vaccination programmes, including TB.
“The impact of flooding on TB is usually seen sometime later, but it, of course, has an immediate impact in disrupting treatment which can lead to problems such as drug-resistant TB,” said Yassin.
TB experts are calling for governments and leaders within the TB community itself to begin paying more attention to the issue and start thinking about current TB programs and where changes need to be made to deal with these potential impacts.
Some groups, like TB Alliance, are looking to mitigate some of these impacts through treatment developments. The group recently developed a new TB treatment regimen, BPaL, with a much shorter treatment length and fewer of the sometimes very toxic side effects of previous regimens.
An oral-only regimen involving only a few pills a day, it has been widely praised by patients and experts for the relative ease with which it can be taken, notably in Ukraine, where it has recently been rolled out programmatically and used among the many millions displaced there because of the Russian invasion.
“What we are focusing on is trying to find solutions to make treatment safer and shorter, which would overcome some of the negative effects of climate change related to TB, for instance, displacement, as there would be less chance of treatment interruption with shorter treatment,” said Beumont.

A doctor studies x-rays of a TB survivor at a clinic in Kyiv, Ukraine. Credit: Getty Images for TB Alliance
Yassin said that investment in health systems, especially in low-income countries which have some of the world’s highest TB burdens and where healthcare is already under-resourced, is also crucial.
“We learnt from Covid that health systems can’t cope with a pandemic, and TB is actually a pandemic. It is very important for countries to think about strengthening their health systems and making them more resilient. There needs to be investment now to prepare the systems for a pandemic, including climate change-driven TB,” said Yassin.
“There was a collapse of some healthcare systems during Covid, and because of that, all resources in some countries went to dealing with that, and TB was forgotten, and the TB burden of those countries rose. We need to invest now, not wait for another pandemic. We need more resources,” he added.
Meanwhile, others say that alongside these measures, individual, non-climate-specific interventions could help.
Dr Krishnan Rajendran of the ICMR-National Institute for Research in Tuberculosis (NIRT) in India, which has the highest burden of TB in the world according to the World Health Organisation, told IPS that lessons learnt from the Covid pandemic could be used to reduce TB spread.
“National and local authorities could take preventive measures, such as at least encouraging people to wear masks in seasons where TB incidence is high,” he said.
Whatever efforts are made to deal with the impact of climate change on the disease, they need to be made soon, said Yassin.
“We shouldn’t wait for climate change impacts [to fuel the spread of TB] before we act—we should do something now and deal with TB to prevent more deaths and disabilities,” he said.
IPS UN Bureau Report